This blog post was written by Prof. Henk van Beijeren and details key ingredients of exit strategies.
In my opinion, an exit strategy ought to consist of two parallel tracks: reducing the number of infected people by maintaining serious lockdown measures to a level where it can be controlled by testing and tracing; and developing a vaccination program as quickly as possible.
Keeping Infections Low
We need to keep infections low in order to avoid overburdening the healthcare system which would lead to unnecessary deaths. The lockdown measures have accomplished this so far, and they must be supported by the following specific measures.
Testing and tracing capacity needs to be enhanced as much as possible; testers and tracers must be recruited and instructed, as waiting for an app to support this would be too risky. However, if an app meeting all requirements will be developed, of course it is very welcome.
All healthcare workers need to be provided with enough protection materials for all healthcare workers, supporting staff and other high risk groups.
As soon as infection levels are down to a level that is manageable for testing and tracing, lockdown measures may be relaxed gradually as levels go down further. Citizens need to understand that this is the fastest way back to normal, and that discipline is crucial. Policy-makers ought to sketch a tentative timeline and outline a perspective for improvement, as this increases understanding and acceptance in the population.
Travelers from abroad ought to be checked and monitored carefully. Medical attests of being free of Covid-19 may be required, tests may be taken on entrance, and quarantine may be requested (and checked!) on suspicion of infection.
Flu vaccines should be given to the whole population. A spread of a flu virus and the novel coronavirus at the same time would be very dangerous, because it makes Covid-19 much harder to recognize and it may overburden testing stations. Mouth masks must be made available to the whole population.
Developing a Vaccination Program
At the same time as infections must be kept low, a vaccination program must be developed at the highest possible speed. This does not necessarily require a vaccine that provides immunity with 99.9 % probability; a vaccine doing so with 70% or even 50% probability is good enough for a first shot. It will provide herd immunity or at least make a large step toward it.
In combination with testing for immunity (hopefully this will soon be possible at large scale!) the vaccination program would strongly alleviate the present economic and societal burden.
Have a rapid, though very careful phase-1-2 study following preliminary registration, and a rapid start of mass production after the phase-1-2 study has established safety and significant antibody production. Start by vaccinating low-risk groups and, in continued absence of negative effects gradually scale up to groups of higher risk.
Easiest to develop would be a vaccine based upon inactivated whole virus in combination with a standard carrier. Absence of adverse effects and sufficient effectiveness would have to be tested for very carefully. Rapid mass production may be possible in facilities used for standard vaccines.
Other vaccines may equally be released and produced already after standing a successful phase-1-2 trial. Vaccine development and improvement must be continued until a fully satisfactory vaccine is available. In China, a successful phase-1 trial has been performed with an inactivated whole-virus vaccine (see Gao et al., 2020).
It is important that the development of vaccines against Covid-19 is not done by industry alone. There must be an impartial and non-bureaucratic authority that stimulates the development of the most successful and rapidly deployable vaccine candidates. In addition, this authority must be able and willing to temporarily relax and speed up registration standards. Dependence on production in a single or just a few countries, which may need the vaccine badly themselves, may be risky and should be avoided if possible.
The Situation in The Netherlands
In the Netherlands the capacity available for testing and contact tracing is probably already sufficient. This may be illustrated by the case of GGD Groningen, which could afford using this protocol thanks to the relatively small number of infections in its region. At the height of the epidemic it handled 26 cases on a single day (March 24, RIVM data) without problem; see the figure below.
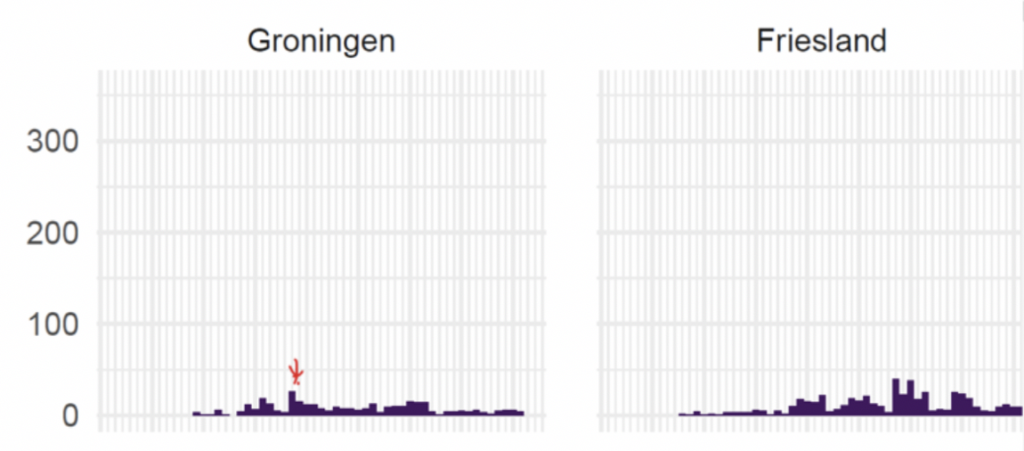
Scaling this up to the size of the full Dutch population (from 584.000 people to 17 million) one may estimate that all GGD’s together could test and trace close to 800 people, and almost certainly even more, on increasing the available work force and amount of testing materials.
The present number of registered new infections during a day is 400 (April 27, RIVM data), so there should not be a problem; see the table below.
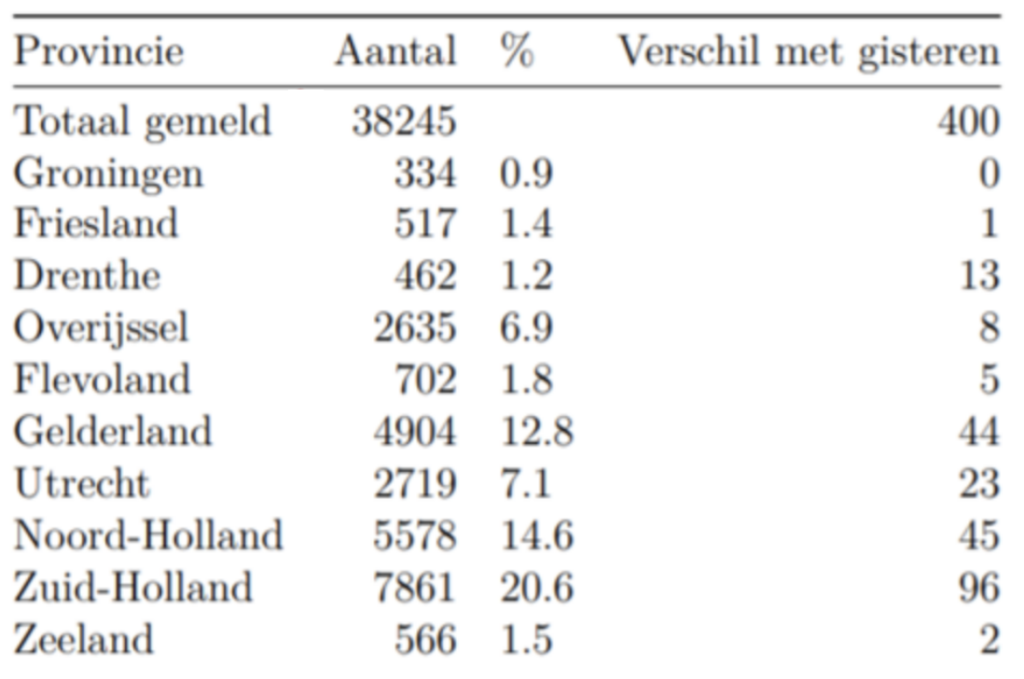
However, strong coordination and flexible and fast reallocations of people, tasks and testing materials will be needed, as the numbers of positively tested persons vary widely among the GGD’s.
To be able to relax lockdown measures one has to simultaneously increase the scale of testing in order to keep the infection coefficient well below unity. Criteria for testing have to be widened, test locations have to be nearby everywhere and the supply of testing material has to be kept up at increasing levels. The amount of contact tracing need not increase, as the number of infected people will keep decreasing exponentially. By carefully managing the relaxation of the lockdown measures in combination with increasing testing, one may speed up this decrease.
On April 23 the number of testing labs in the Netherlands was reduced from 40 to 30. This is not the right policy. Rather, if fewer tests are needed for the groups tested presently, the scope of testing and contact tracing has to be extended. By lack of a vaccine this is the only way to arrive at an acceptable relaxation of the lockdown measures.
Relaxing the lockdown measures could be done at a different pace in different regions, depending on local infection densities.
Almost zero infection rate may be reached and maintained by using very severe testing criteria and very good screening of travelers from abroad. Presently, Taiwan may be the best example of this.
It would make sense weighing the risk of starting vaccination already after successful completion of a phase-1-2 testing program against that of not vaccinating and maintaining the risk of catching the disease. The outcome may depend on country and risk group. Experiences gained with vaccination in one country can be used in other ones. An interesting idea is that of having volunteers being infected with Covid-19, after receiving an experimental vaccine and undergoing a test for antibody production (see Callaway, 2020).
It would be advisable to test both terminal patients (if possible, all of them) and recovering ones for amounts and types of antibodies they produced. This way it may be possible to identify a “safe” level above which no casualties were found. By lack of better methods this could serve as an indirect proof of immunity.
The search for medicines must be continued at great speed. But also with care and without bias. We should never fall into the chloroquine-azithromycin trap again (it has now been shown in two trials that this combination is dangerous).
Conclusion
In this post, I have outlined two key lines a successful exit strategy should follow in parallel: extensive testing and contact tracing to keep infections low as we slowly lift the lockdown; and the development of a vaccination program, which is sped up by slightly relaxing the strict requirements vaccines usually have to fulfill.
An important conclusion is that in all likeliness the Netherlands already have the capacity for containing the disease by testing and tracing; this just has to be mobilized, organized, and perhaps extended somewhat by recruiting and instructing testers and tracers.
Generally, one should keep an open eye for what happens in other countries, learn from them, and adopt measures with positive effects while avoiding negative or useless ones.
Most importantly, we must have world class leadership.